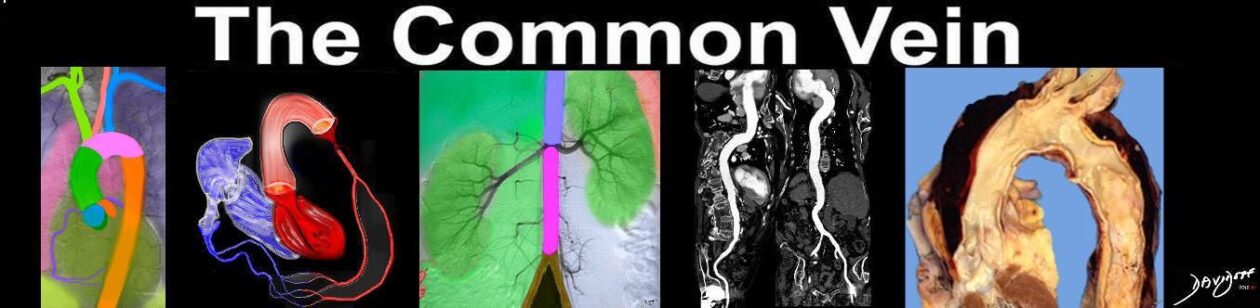
FUNCTION
The Common Vein Copyright 2007
Ashley Davidoff MD
Cristina Cesaro
Introduction
The aorta’s tubular structure and elastic nature gives rise to its specialized function as a transporter of oxygenated blood to the tissues of the body. The aorta’s strong and elastic walls enable it to transport blood under high pressure to the peripheral tissues. As the first receptor of newly oxygenated blood from the heart, it is the aorta’s function to accommodate the stroke volume, process it by the basic mechanisms of fluid transport, and to export its flow in such a manner that can efficiently support the tissues’ metabolic needs. The aorta helps control the rate of blood perfusion by regulating pressure and blood velocity. Its structure employs these specialized properties by mostly mechanical means and minor chemical forces. These forces arise from the aorta’s ability to create and maintain pressure gradients by its elastic and tubular form innervated by sympathetic tone. The interactions between the mechanical forces of elasticity and strength are most essential, especially during resting conditions.
Principles
Introduction
The aorta’s physiology executes its biological function of transport. As a large and elastic tube attached to the heart, the aorta receives and transports cardiac output. All the while, the aorta operates under high pressures to ensure blood flow is fast and efficient. The aorta primes the beginning journey of blood through the systemic circulation which feeds our bodily tissues. By mechanical and chemical means, the aorta helps fulfill their individual metabolic needs so that our body can function while appropriately adapting to changes in the external environment.
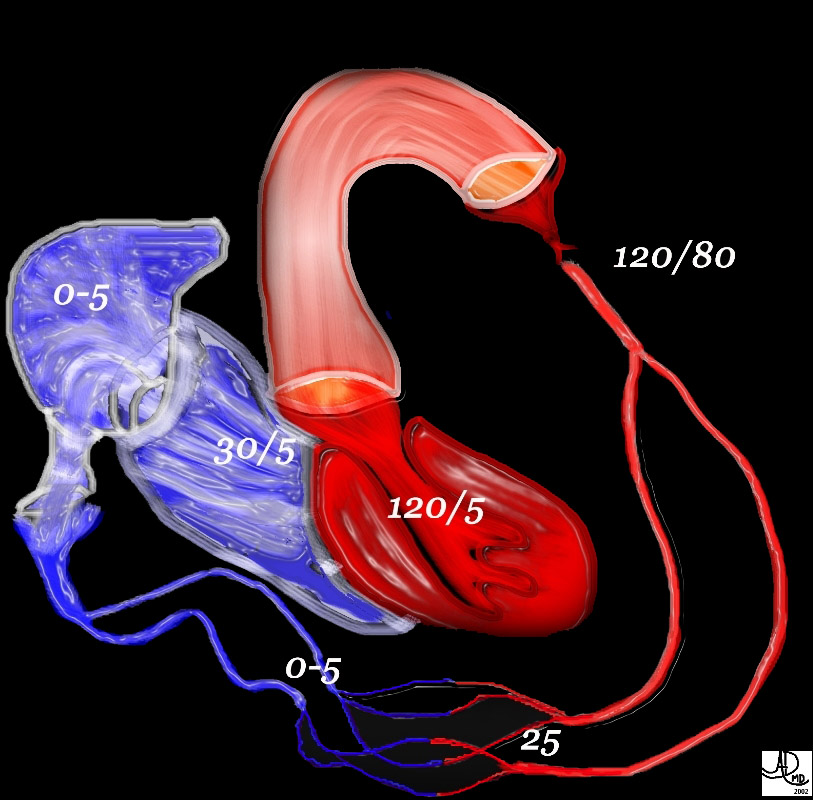
49483b01
key words
heart cardiac LV left ventricle aorta aortic systemic circulation capillary capillaries arterioles venules right atrium RA right ventricle RV normal physiology pressures hemodynamics
Ashley DavidoffForces
Mechanical
The aorta’s mechanical forces, arising from its physical makeup, contribute greatly to its primary function of transport. Its elasticity and strength are the most valuable physical characteristic of the aorta, mechanically interacting in the transportation of blood under high pressures. In concert, the aorta is able to stretch when blood enters, but is strong enough to do so gradually so that pressure does not rapidly drop. This provides fast flow through the systemic circulation. Without these mechanical properties, the aorta would simply be a rigid tube; just a pathway for blood. The interaction between elasticity and strength defines its primary function of transport in the cardiovascular system.

The lumen (red) is lined by the endothelium (thin pink layer) followed by the (teal) media which is mostly elastic tissue, and then by the adventitia (thick pink). Courtesy of: Ashley Davidoff, M.D. TheCommonVein.net aorta Philips 003
Chemical
In addition to the mechanical transportation of blood, the aorta occasionally functions according to the chemical forces governed by the nervous system. Within the aortic adventia is a network of nerves containing mostly adrenergic fibers. Nervous control enacts through both chemo- and presso-receptors embedded in the aortic wall, most of which are located in the aortic arch. These fibers cause the aorta to contract or dilate by sympathetic response, regulating the force of blood flow alterations in pressure. The chemical receptors react by humoral control governed by the adrenal medullae. According to the body’s activity in relation to the environment, different neurotransmitters are released into the blood. Those that initiate contraction of the walls are vasoconstrictors while vasodilators initiate the opposite. Pressoreceptors or baroreceptors embedded in the aortic wall causing contraction or dilation in a different manner. They are activated by a physical stretch in the aortic wall. In turn, the baroreceptors initiate a stretch reflect transmitted through Hering’s nerves to the glossopharyngeal nerves of the neck into the medullary region of the brain. Here, they are processed and signals initiating contraction are returned to the aortic wall and thus carried out.
Interactions
Aortic blood flow is locally controlled by both physical and chemical forces contributed by its overall structure. Under resting conditions, the rate of blood flow is governed mostly by mechanical means. The aorta transports blood by maintaining a pressure difference along its course by its elasticity and radial strength. When the sympathetic nervous system is stimulated, chemical control takes charge of the mechanical forces by inducing contraction or dilation. The aortic arch in particular contains the majority of chemo-receptors which can be stimulated by humoral control. The release of norepinephrine from the adrenal glands causes slight vasoconstriction. Constriction of the aortic walls causes increased pressure and thus increased blood flow. The release of this neurotransmitter is the body’s physiological response to a change in their environment, such as increased stress due to exercise. The aorta’s pressor receptors, specifically called baroreceptors, also act in overlap with such a change. An increase in blood volume causes an increase in pressure, which initiates the stretch-induced vascular depolarization of the baroreceptors. This causes myogenic contraction of the aortic tissue, which in turn increases blood flow.
Receive Process and Export
The aorta receives the cardiac output of the heart. Cardiac output regulation is the sum of blood flow participating in tissue metabolism of the body. It changes depending upon the rate of each tissue’s metabolic needs. In general, it is the amount of blood the aorta receives per minute which then must be processed by transport. Under resting conditions, the heart normally pumps about 5 L/min into the aorta. At increasing levels of activities, the output increases proportionally to perform the work needed. It is the aorta’s job to adapt to the body’s varying metabolic needs, and thus changes in cardiac output. During resting or non stressful conditions, the aorta governs the rate of blood flow by mostly mechanical means. It maintains a steady high pressure during systole and diastole so that blood can be pushed through the ventricle and properly received by the aorta. Its ability to maintain a pressure gradient between the left ventricle and itself allows blood to quickly enter and begin its flow.
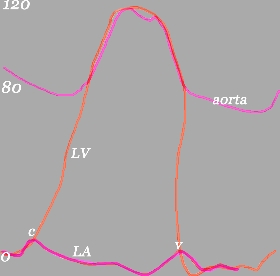
Aortic Pressure LV Pressure and LA Pressure |
| This image shows the pressure waves of the LV,(orange) aorta (light pink) and left atrium. (dark pink) The LV pressures start with the steep rise of systole , and a rapid dramatic steep fall to very low pressures during diastole. The aorta follows the LV with a steep rise, but during diastole, the elastic recoil aided by the peripheral resistance enables a steady maintenance of diastolic pressure in the aorta of about 80 mmHG.(upper pink) |
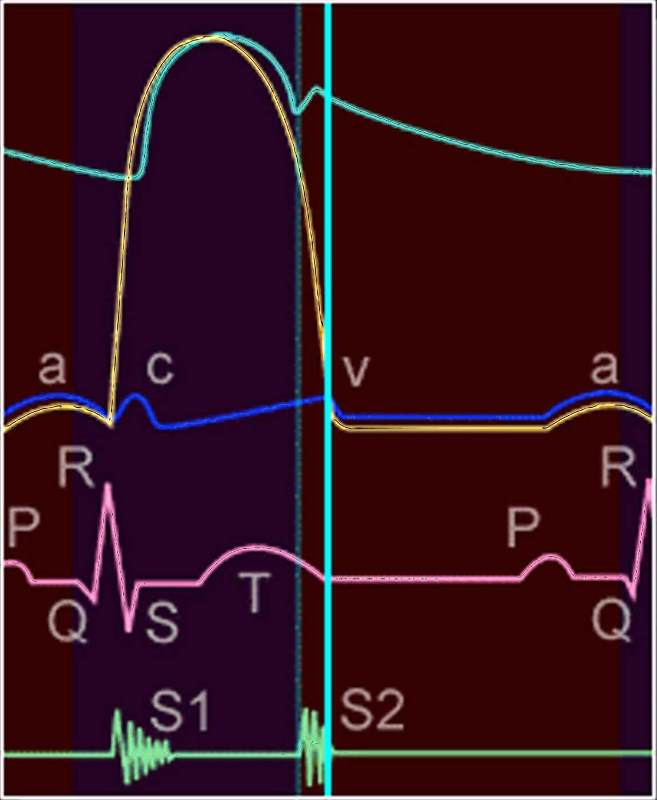 Wigger’s Diagram of a Single Heart Beat Wigger’s Diagram of a Single Heart Beat |
| 33808b.800 heart cardiac physiology pressure EKG ECG pressure curves diagram LV aorta LA left atrium left ventricle systole diastole acv waves Davidoff MD |
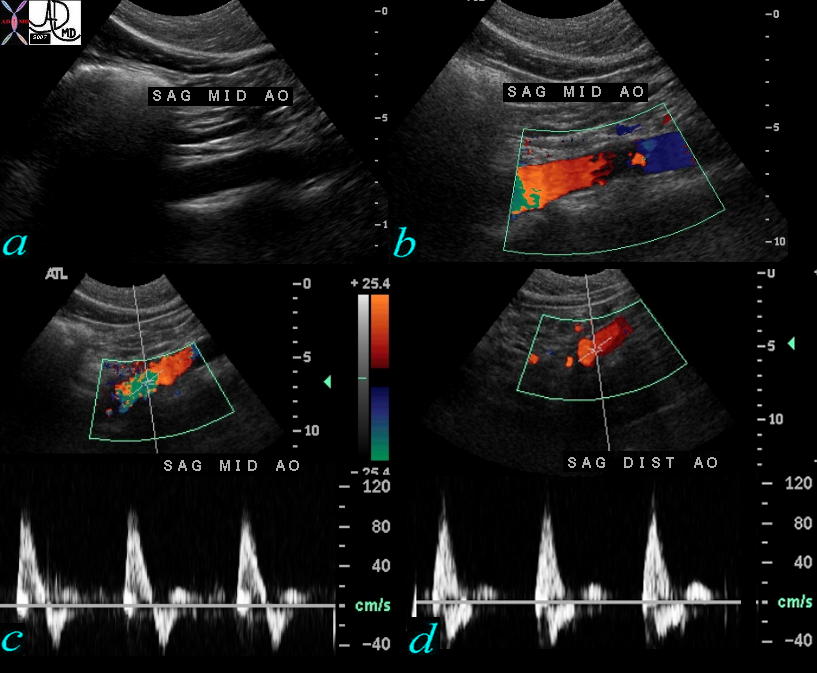 Laminar Flow and Velocities in Abdominal Aorta Laminar Flow and Velocities in Abdominal Aorta |
| 73394c01 aorta abdomen abdominal aortic flow velocity laminar flow a = gray scale b = doppler color flow showing laminar flow c = velocity in proximal abdominal aorta d = flow velocities in distal abdominal aorta normal physiology USscan doppler Davidoff MD |
The aorta then processes the blood by transport. It accomplishes this primary function by both mechanical forces and occasionally chemical forces. Once blood has entered the aorta, its vascular walls stretch so that the pressure increases accordingly (approximately 120 mmHg). An increase in pressure causes an increase in blood flow which propels the blood into the branching arteries along its course. These branches distribute the blood to their respective locations throughout the body. Pressure then falls gradually, again doing so by its elastic nature. A slow decrease in pressure allows the left ventricle to easily eject blood while maintaining a high pressure environment needed to ensure a high blood flow velocity. If cardiac output rapidly increases from its normal rate, chemical forces governed by the sympathetic nervous system enhance the aorta’s natural ability to dilate and contract.
Blood can then be exported or distributed in relation to the body’s needs. The branches of the aortic arch nourish the upper regions of the body while the lower branches perfuse the peripheral organs. All of these functions—receiving, processing and exporting—are constantly being performed in accordance to the body’s ever-changing needs. For example, while exercising, the body’s tissues are metabolizing at a higher rate. The aorta then must adapt its functions in correlation with an increase in muscle activity occurring at the cellular level. Blood is received at a higher volume, processed by a greater and more appropriate force, and then exported efficiently to the proper tissues affected by such a change.
Protection
The aorta’s strong and elastic vascular walls protect the aorta from shear stress caused by angular blood flow and high pressures. The aortic endothelial cells of the wall can withstand the ejection force of pumped blood by stretching and recoiling in a pulsatile fashion. Each cell contains the fibrous protein actin, structurally assembled parallel to the aortic wall. These essential proteins functions as stress fibers. Upon stretching, the actin absorbs the perpendicular pressure applied by each ventricular ejection and recoils in a feedback control method. Its specific orientation within the endothelial cells reduces the force of external stress.
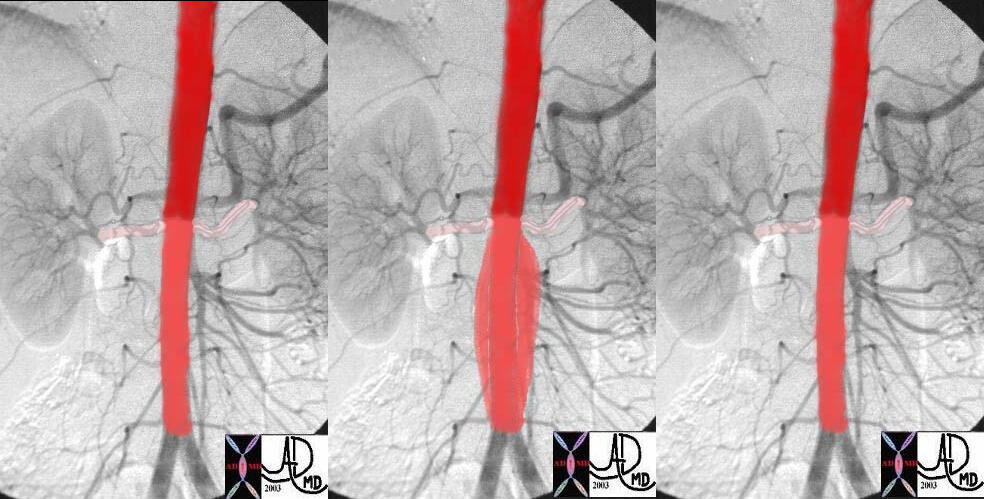
Systole and Diastole in the Elastic Aorta |
| This image of the theoretical functioning of the role of resistance and outflow enabling the infrarenal aorta to function as second pump. In systole (b) the suprarenal artery is expanded by the pulse but is relatively decompressed by the the low resistance and high flow renal arteries. The infrarenal aorta is relatively more expanded in systole (b) since the iliac arteries offer a relative resistance. This increased resistance causes the elastic tissue in the aorta to stretch (b) so that the recoil in diastole (c) results in a sustained forward moving force assisting the blood to get to their most distal destination – the feet. Courtesy Ashley Davidoff MD. 24877c |